Monthly Archives: December 2024
World’s oldest-known wild bird lays an egg in Hawaii at age 74
By
Published Dec. 6, 2024
Updated Dec. 6, 2024, 3:46 p.m. ET21 Comments
4 seconds of 54 secondsVolume 0%
This bird’s no spring chicken — but she’s procreating in her 70s!
The world’s oldest known wild bird, an albatross named Wisdom, triumphantly laid her first egg in years this week at the ripe old age of 74.
“We are optimistic that the egg will hatch,” Jonathan Plissner, supervisory wildlife biologist at Midway Atoll National Wildlife Refuge in Hawaii said.


The video player is currently playing an ad.Skip Ad
The long-winged seabird popped out the potential baby near the Hawaiian Archipelago islands after returning there with her mate earlier this week.
The frisky fogey and her life-long lovebird, Akeakamai, had flown back to the circular chain of reef islands to lay and hatch eggs since 2006.
But Wisdom hadn’t laid an egg in four years after Akeakamai apparently flew the coop and disappeared several years ago.
Wisdom was later seen interacting with another male before she recently reunited with her long-term mate.
The bird — who has laid an estimated 60 eggs in her life — was first banded as an adult in 1956 and has raised as many as 30 chicks, Plissner said.
The average lifespan of a Laysan albatross, which mate for life, is 68 years, according to the National Oceanic and Atmospheric Administration.


The age at which the birds stop laying eggs in the wild hasn’t been effectively studied and is unknown.
Every year, millions of the seabirds return to the refuge to nest and raise their young and their chicks fly out to sea about five to six months after hatching.
Body of Shelby County Coroner discovered in Lake Mattoon in hunting accident
What to Know About the Bird Flu amid the Current Outbreak
Concern grows over whether bird flu could lead to a pandemic: What to know
The virus has been found in raw milk, deepening concerns about bird flu spread. Experts discuss the symptoms and how to prevent getting sick.
0 of 30 secondsVolume 0%
This ad will end in 26
Anniversary of Pearl Harbor marked with ceremonies in Hawaii
Create your free account or log in to save this article
Dec. 6, 2024, 8:33 AM PST / Source: TODAY
By A. Pawlowski
H5N1 bird flu, a type of avian influenza, has infected dozens of people in the U.S., and spread to seven states and Canada this year.
As concern grows over whether it could lead to another pandemic or lockdown, California has announced a broad recall of raw milk and cream after the virus was found in some of the dairy.
ADVERTISING
There have been 32 human cases of bird flu in California this year — including the first U.S. child — according to the CDC. (None are linked to raw milk.) There have been 58 in the U.S. in total.
Almost all human bird flu patients have had contact with infected animals, but three cases in North America are getting particular attention because it’s not known how they were exposed to the virus: the child in California, a teenager in Canada and a person in Missouri.
The Canadian teen remained in critical condition at the end of November, weeks after symptoms started, and was being treated for acute respiratory distress at a children’s hospital in British Columbia after testing positive for H5N1 bird flu, the country’s first human case, the CBC reported.
The patient “was a healthy teenager prior to this” with no underlying conditions, the province’s health officer, Dr. Bonnie Henry, said in a news conference.
The young person’s deterioration was “quite rapid,” Henry said.
“It reminds us that in young people, this is a virus that can progress and cause quite severe illness,” she noted.
Could bird flu cause the next pandemic? Here’s what to know about raw milk and bird flu, symptoms, how to protect yourself and more.
Raw milk recall amid bird flu outbreak
The recall was implemented after “multiple bird flu virus detections” were found in products from Fresno’s Raw Farm, LLC, the California Department of Public Health announced.
All sizes of Raw Farm milk and cream produced between Nov. 9 and Nov. 27, have been pulled from store shelves, according to the notice. The affected lot numbers are 20241109 through 20241127.
The California Department of Public Health has also placed the farm under quarantine.
While the recall only applies to raw whole milk and cream, the agency urged people to also avoid consuming the company’s cheese and kefir, and avoid raw milk pet food topper and pet food kefir marketed to pet owners.
There are no reports of anyone getting sick, but consumers “should immediately return” any of the recalled products they may have in their fridge, the agency added.
California is the epicenter of the current outbreak of H5N1 in dairy cows, Meghan Davis, an associate professor of environmental health at the Johns Hopkins Bloomberg School of Public Health, told NBC News.
Raw milk, which is not pasteurized, can expose people to germs and lead to serious health risks, the Centers for Disease Control and Prevention has warned.
Consumers don’t realize the raw milk they buy is not from a single cow, but pooled from many cows, says Dr. Ian Lipkin, an expert on emerging viral threats.
“If one cow in that group has H5N1, then it gets distributed to many, many more people,” Lipkin, professor of epidemiology at the Columbia University Mailman School of Public Health, tells TODAY.com. “It’s not a good situation.”
Drinking or accidentally inhaling raw milk containing bird flu virus may lead to illness, California health officials warn. So can touching your face after touching the contaminated milk.
Pasteurized milk is safe to drink because pasteurization kills the bird flu virus and other germs, the experts emphasize.
What is bird flu?
Like people, birds can get the flu, and the avian influenza viruses that make birds sick can sometimes infect other animals like cows and, rarely, people, the National Library of Medicine explains.
H5 is one family of bird flu viruses. It has caused widespread flu in wild birds worldwide and is causing outbreaks in poultry and U.S. dairy cows, the CDC notes. Some farm workers exposed to those animals have also gotten sick.
H5 has nine subtypes, including H5N1, the strain responsible for the recent illnesses.
Which states have human cases of bird flu?
There have been 58 confirmed human cases in seven states in the U.S. during the 2024 outbreak, according to the CDC.
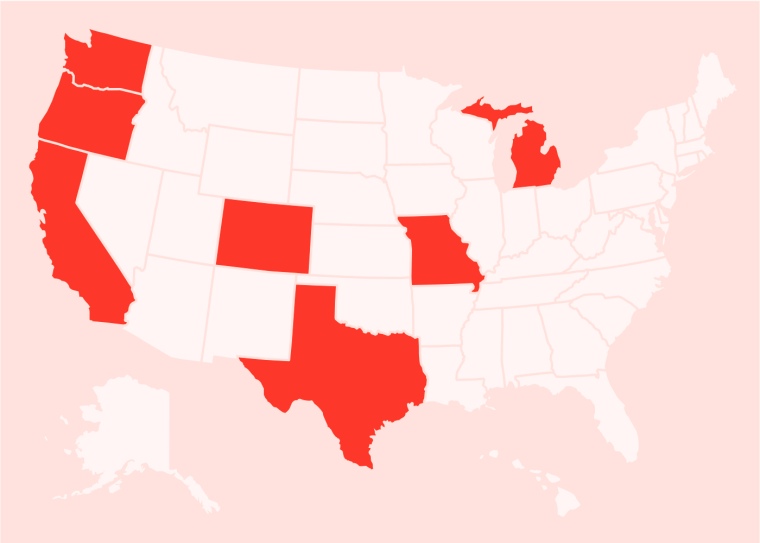
They’ve been reported in:
- California: 32 cases
- Colorado: 10 cases
- Michigan: 2 cases
- Missouri: 1 case
- Oregon: 1 case
- Texas: 1 case
- Washington state: 11 cases
Recommended

Gift Guides36 stimulating gifts for seniors who are still young at heart

Lifestyle & FitnessThis affordable rower is helping me get a head start on my 2025 fitness goals
Almost all U.S. patients had contact with infected cattle or poultry. The two exceptions — a patient in Missouri and a child in California — had no known animal exposure.
There’s been no confirmed person-to-person spread.
Bird flu outbreak 2024
“We do have an outbreak of human infections of H5N1,” says Dr. Amesh Adalja, a senior scholar at the Johns Hopkins Center for Health Security and a spokesperson for the Infectious Diseases Society of America.
The current public health risk from H5 bird flu is low, the CDC says. Its flu monitoring systems currently show no signs of unusual flu activity in people, including the H5N1 virus, or any unusual flu-related trends in emergency department visits.
But the agency is “watching the situation carefully” — as are experts in the field.
Lipkin calls it an important health concern.
“Emerging infectious diseases are unpredictable. If you told me 20 years ago that we were going to have major problems with coronaviruses, I wouldn’t have predicted that,” Lipkin says.
“So nobody knows what’s going to happen with this particular flu.”
Human infection with bird flu can happen when virus gets into a person’s eyes, nose or mouth, or is inhaled, according to the CDC. The illness can range from mild to severe and can be deadly.
Human H5N1 cases in the U.S. have been relatively mild, perhaps because people are mostly getting infected through their eyes, Adalja notes.
It might happen when a dairy worker is milking an infected cow and gets squirted in the face with the milk, for example.
“You’re getting infected from the eyes rather through the respiratory route,” Adalja tells TODAY.com. That may be “less risky than respiratory inhalation” of the virus, he adds, when it can go to the lungs.
Is bird flu a global health emergency?
No, the World Health Organization doesn’t currently categorize the bird flu outbreak as a global health emergency. Outbreaks that do fall into this category include COVID-19, cholera, dengue, Marburg virus and mpox.
Could bird flu turn into a pandemic?
Experts say it’s unlikely this particular strain of bird flu would lead to a pandemic because it doesn’t have the ability to spread efficiently between people.
H5N1 has been infecting humans since 1997, so it’s had time to evolve, but still doesn’t easily jump from person to person, Adalja points out.
“I don’t think that this is the highest risk bird flu strain,” he says. “You can’t say the risk is zero. But of the bird flu viruses, it’s lower risk.”
Lipkin had a similar take.
“Nobody ever wants to say never because you can be wrong,” he cautions. “Could this virus evolve to become more transmissible? Yes. Has it done so thus far? No. Do I personally think it’s going to be responsible for the next pandemic? No. Could it be? Yes.”
One concerning development is that a pig in Oregon tested positive for H5N1 in October — the first time the virus has been detected in swine in the U.S., NBC News reported.
It’s worrisome because pigs can become infected with both bird and human viruses at the same time, allowing mutated strains to emerge.
“Pigs are considered a mixing vessel for flu viruses. So we always worry when a pig gets infected with a bird flu strain because pigs can also be infected with other strains,” Adalja says.
“Those strains can all recombine in the pig as a mixing vessel and then something different will come out.”
Since there are many different avian influenza strains, one of them may be able to cause a pandemic at some point in the future, Adalja adds.
The bird flu strain he’s more worried about as a pandemic risk is H7N9, which was first reported in humans in China in 2013 and expanded to more than 1,500 people by 2017. This virus also doesn’t spread easily from person to person, but when people do get infected, most become severely ill, the World Health Organization warns.
The most recent human H7N9 virus infection was reported in China in 2019, according to the CDC.
Could there be a lockdown due to bird flu?
A lockdown due to bird flu is not likely for this strain, since H5N1 isn’t posing a threat to the general public, both experts say.
If that were to change, people should realize lockdowns, like those during COVID-19, are not the “go-to measure” for an infectious disease emergency, Adalja says, calling them “very blunt tools.”
Instead, proactive measures — such as more aggressive testing of farm animals — will allow health officials to be much more precise when it comes to stopping the spread of infection, he notes.
When it comes to lockdowns, there’s also the question of how far authorities are willing to go.
“If H5N1 were to become a major health problem, we would have to talk about (containment),” Lipkin says. “But I don’t think that this incoming administration is going to be amenable to that.”
What is the treatment for bird flu?
It’s oseltamivir, also known as Tamiflu, the same antiviral medication used for ordinary cases of flu.
It’s important to start that drug as soon as possible after symptoms start for it to have impact, Lipkin says. Some close contacts of people who’ve been infected with H5N1 have also received the drug as a precautionary measure to prevent infection.
Is there a bird flu vaccine?
Four vaccine candidates for dairy cows have been approved for field trials, according to the U.S. Department of Agriculture.
In poultry, four potential bird flu vaccines began to be tested in 2023, Reuters reported.
When it comes to humans, the CDC says the U.S. government is developing vaccines against H5N1 viruses “in case they are needed.”
The agency adds it has H5 candidate vaccine viruses that could be used to produce a vaccine for people, and preliminary analysis shows “they are expected to provide good protection” against H5N1.
There are also some vaccines in the strategic national stockpile that are closely — if not exactly — matched to this particular strain of bird flu, Adalja says.
“There are efforts to make more updated vaccines. But there is no widespread vaccination program being initiated against H5N1 at this time in the U.S.,” he notes.
In the summer of 2024, Finland became the first country in the world to offer bird flu vaccinations for people at risk of exposure, including workers at fur and poultry farms.
Finland bought vaccines for 10,000 people, each requiring two injections, Reuters reported.
In December 2024, the United Kingdom announced it has secured more than 5 million doses of human H5 influenza vaccine. The purchase will “boost the country’s resilience in the event of a possible H5 influenza pandemic,” the UK Health Security Agency said in a statement.
What does bird flu do to humans?
Bird flu in humans can cause no symptoms, or anywhere from mild to severe symptoms, according to the CDC. Most people who have been infected with bird flu have reported mild symptoms, such as eye infections and flu-like symptoms, according to Yale Medicine.
The CDC lists the following bird flu symptoms:
- Eye redness
- Mild flu-like upper respiratory symptoms
- Fever or feeling feverish
- Cough
- Sore throat
- Runny or stuffy nose
- Muscle or body aches
- Headaches
- Fatigue
- Shortness of breath or difficulty breathing
- Pneumonia requiring hospitalization
- Diarrhea, nausea, vomiting or seizures (these are less common symptoms).
H5N1 mortality rate
The mortality rate of bird flu in humans, based on the roughly 900 confirmed people infected with the virus between 2003 and 2024, is about 50%, according to Yale Medicine.
However, it’s likely that many more people have been infected without knowing it because they had no or mild symptoms, so the mortality rate could be much lower than 50%. And the mortality rate would likely drop even further if treatment and vaccines were made more wildly available, should human-to-human spread start to occur.
How do you get bird flu?
There are several ways the bird flu virus can spread from animals to people, according to the CDC:
- Touching something contaminated with the virus and then touching your nose, eyes or mouth
- A liquid that contains bird flu virus splashing into your eyes (such as raw milk from an infected cow)
- Eating, drinking or breathing in droplets containing the virus
How to protect from bird flu
The people most at risk for H5N1 bird flu are dairy and poultry workers who might be around infected animals, Adalja says. They should wear personal protective equipment while working on farms affected by the virus, the CDC advises.
When it comes to the general public, “don’t consume raw milk, full stop” since H5N1 is viable in it, Lipkin says. Pasteurized milk can eliminate the risk of infection, he notes.
Properly cooked chicken is safe to eat, but wash your hands with soap and water after handling raw chicken, he adds.
It might be wise to skip petting zoos or events where you can learn how to milk a cow, Adalja adds.
Avoid direct contact with sick or dead wild birds, poultry and other animals, the CDC advises.
H5N1 bird flu is closer to gaining pandemic potential than we thought
How Much Of A Risk Is Bird Flu? Study Raises Fears For Humans
Why hasn’t the bird flu pandemic started?
Some scientists examining mutations found in H5N1 viruses fear major outbreak is imminent but others say pathogen remains unpredictable
- 5 Dec 2024
- 6:40 PM ET
- ByKai Kupferschmidt
Share:
Related article
From bad to worse: How avian flu must change to trigger a human pandemic
BY Kai Kupferschmidt
News
06 Apr 2023
If the world finds itself amid a flu pandemic in a few months, it won’t be a big surprise. Birds have been spreading a new clade of the H5N1 avian influenza virus, 2.3.4.4b, around the world since 2021. That virus spilled over to cattle in Texas about a year ago and spread to hundreds of farms across the United States since. There have been dozens of human infections in North America. And in some of those cases the virus has shown exactly the kinds of mutations known to make it better suited to infect human cells and replicate in them.
No clear human-to-human transmission of H5N1 has been documented yet, but “this feels the closest to an H5 pandemic that I’ve seen,” says Louise Moncla, a virologist at the University of Pennsylvania. “If H5 is ever going to be a pandemic, it’s going to be now,” adds Seema Lakdawala, a flu researcher at Emory University.
Others are more sanguine, noting that similarly menacing avian flu viruses, such as one called H7N9, have petered out in the past. “Why didn’t H7N9 end up being easily human-to-human transmissible and cause a pandemic?” asks Caitlin Rivers, an epidemiologist at the Johns Hopkins Center for Health Security. “I feel like there’s really no way to estimate and it could go either way.”
SIGN UP FOR THE AWARD-WINNING SCIENCEADVISER NEWSLETTER
The latest news, commentary, and research, free to your inbox daily
Ever since H5N1 first caused an outbreak in humans in Hong Kong in 1997, sickening 18 who had been in contact with infected poultry and killing six, the avian virus has been high on lists of potential pandemic agents. Scientists have since built up a picture of the minimum changes H5N1 likely needs to spread widely in humans: mutations in its polymerase, the enzyme the virus uses to copy its genome, and in its hemagglutinin—the H in H5N1—the protein the virus uses to attach to cells, to stabilize it for airborne transmission and help it better bind to cells in the human upper airways.
A slew of recent findings all seem to suggest the risk of the current H5N1 clade in cattle and birds causing a pandemic is actually higher than previously thought. A study looking at blood samples from workers at H5N1-infected dairy farms in Michigan and Colorado found that many human infections go undetected, each one offering the bovine virus more chances to adapt to us. A preprint out this week indicates currently circulating clade 2.3.4.4b viruses are better at binding to human epithelial cells in the airways than previous versions of H5N1. And a Science paper out today shows in lab studies that a single mutation at one hemagglutinin site, dubbed 226L, is enough to shift the virus’ preference from the avian-type cell surface protein to human-type receptors. Many scientists had thought at least two mutations were required. A switch based on just one mutation “means the likelihood of it happening is higher,” says Jim Paulson of Scripps Research, one of the authors.
So why hasn’t H5N1 touched off a pandemic yet?
Advertisement
One simple answer is that the virus may just need more time to hit the right combination of mutations. The high mutation rate of influenza viruses should tip the odds in H5N1’s favor: “My rule of thumb is that one in 4000 [virus] particles will have a mutation at the amino acid that you are interested in,” Paulson says. Indeed, one polymerase mutation the virus likely needs, dubbed 627K because it leads to the amino acid lysine (K) at position 627 of the protein, has been found several times in strains infecting mammals but also in virus isolated from the first human case associated with the U.S. outbreak in dairy cows.
On the other hand, the viruses in birds, cattle, and people so far show no signs of the 226L hemagglutinin mutation that would allow H5N1 to better latch onto human receptors. Researchers speculate that change might hamper the virus in some way, and a second mutation may be needed to offset its disadvantages. The two mutations might also have to come in a particular order. “It’s like a dial on a bank vault: You go to the right, then you go to the left, then you go to the right and you’ve got to get a certain number every time,” says Mike Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota Twin Cities.
Dangerous steps
For the H5N1 influenza virus to spark a human pandemic, its genome must acquire mutations that alter several of its proteins. Some have now been seen in viruses infecting people, but none of those appear to have transmitted onward.C. Bickel/Science
In fact, some researchers thought the virus might just be unable to swap an amino acid at position 226 outside the lab. But then came the mysterious case of a severely sick teenager in Canada who has been hospitalized with H5N1 since early November. Virus sequences from that patient suggest some H5N1s had changed the amino acid at position 226 whereas others had not, says Jesse Bloom, an evolutionary biologist at the Fred Hutchinson Cancer Center. “It looks like during the infection of this individual, the virus could have been evolving towards at least some of the mutations that would adapt it to humans.”
This was not the feared 226L mutation: The amino acid had changed to a histidine instead of leucine. Still, “It showed that those sites are mutable in these viruses,” says Tom Peacock, an influenza virologist at the Pirbright Institute. And the glutamine substitution, together with another mutation in the same virus at position 190, could have the same effect as the 226L. For Peacock and others, the finding upped concern about an imminent pandemic.
Unusual factors may have been at play in the Canadian case. The teenager first sought care on 2 November for an eye infection and cough and fever and was hospitalized the week after, when symptoms worsened. The protracted illness may have played a role in the hemagglutinin change, allowing the virus time to hit on a winning mutation. Perhaps more important, the teenager’s virus is the variety that is currently circulating in birds, not cattle. The bird virus, designated D1.1, has clearly gone through reassortment, a mixing of different viruses, presumably in a bird infected with two different avian influenza viruses. In the process it acquired a new neuraminidase, the N in H5N1 and the protein the virus uses to detach new virus particles from the cell that produced them.
Some researchers believe a specific neuraminidase and hemagglutinin combination is crucial to the virus’ success. The two proteins have opposing effects on the same sugar chains on the surface of human cells: Hemagglutinin attaches to these chains, helping the virus infect new cells, whereas neuraminidase cuts those chains, freeing newly formed virus from host cells. “If your hemagglutinin is too sticky and your neuraminidase is too poor, you get stuck to the cell that you’ve just budded from,” Peacock says. If the balance skews the other way, the virus can’t infect new cells.
In the H5N1 variant now circulating in cattle the two proteins may be so well matched that any change in the hemagglutinin is a dead end because it makes the virus much worse at infecting cells. But the newly combined genotype of the bird strain that infected the teenager may have more flexibility to transform into a pandemic virus, says Richard Webby, an avian influenza researcher at St. Jude Children’s Research Hospital. Osterholm agrees. “The cattle one seems pretty stable and could go on like that for a while,” he says. “D1.1 is the one I worry about.”
It is possible that researchers have not yet identified some other crucial change the virus needs to transmit well from humans to humans, Paulson says. “When you do have a pandemic virus, which is very rare, the barrier that that you can identify as having been overcome may not be the only barrier,” he says. “You might be unaware of five or six others that were also overcome at the same time.”
Or, more disturbingly, the virus in the Canadian teenager might actually have had all it needed to go pandemic if only more people had been exposed to it, says viral immunologist Scott Hensley of the University of Pennsylvania’s Perelman School of Medicine. “At the end of the day, I think it is a numbers game.”
